Disc Herniation Explained: Early Symptoms, Daily Triggers, and Prevention
- Dec 14, 2025
- 3 min read
In a work culture that rewards endurance, there are initial signs the body experiences that are often dismissed. Work continues, and posture is adjusted briefly. But when symptoms persist or begin to travel, a phenomenon known as radiculopathy, the body may be pointing to something. One common cause is disc herniation.
What Is the Meaning of Disc Herniation?
Your spine is a sophisticated structure made up of bony segments, called vertebrae, stacked one upon the other. Between these vertebrae sit the intervertebral discs. These critical structures function like shock absorbers and specialized spacers, allowing for movement and absorbing compressive forces.
Each disc is engineered with a tough, fibrous outer layer (the annulus fibrosus) and a softer, gel-like inner core (the nucleus pulposus) that helps the spine stay flexible. How does disc herniation occur?
Disc herniation occurs when the outer layer weakens or tears, allowing the soft inner core to push outward, or bulge. When this displaced material or the inflammation it causes presses upon or irritates a nearby spinal nerve root, characteristic symptoms appear. This can happen in the cervical spine (neck) or the lumbar spine (lower back), depending on where the cumulative strain has built up.
An easy way to picture this is to imagine a sealed sachet of water placed under a heavy book. If the pressure is spread evenly and released often, the sachet holds up well. But if pressure keeps coming from the same spot day after day, the sachet begins to bulge on one side. It does not burst immediately. It gradually loses its shape. That repeated pressure is what prolonged sitting, poor posture, and limited movement can do to the discs over time.

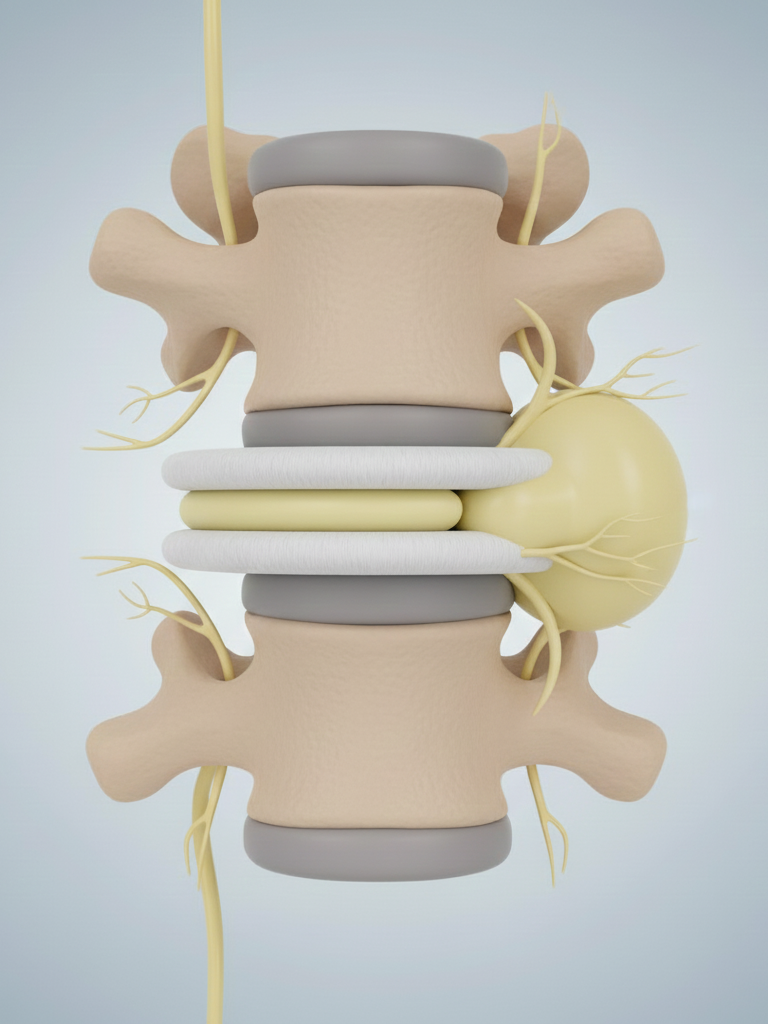
Symptoms That Need Attention
Disc herniation does not always cause immediate or severe pain; in fact, some individuals may have disc changes without any symptoms at all. When symptoms do appear, however, they often follow a recognizable pattern indicative of nerve involvement. These include:
Local pain: It is a persistent pain in the neck or lower back, often worsening after long periods of static posture (like sitting).
Radiating pain (Radiculopathy): It is a pain that travels down the arm or leg. This sensation can be described as sharp, burning, electric, or deep ache, often extending into the hand, fingers, foot, or toes.
Sensory changes: Pins and needles, tingling, numbness, or a feeling of heaviness or deadness in the extremities.
Weakness: A measurable loss of muscle strength, making routine tasks, such as lifting an object or walking on your heels, suddenly harder than usual.
Symptoms often fluctuate with posture. Sitting for extended durations, repeated forward bending, or staying in one prolonged position can increase discomfort. These signs suggest nerve root irritation and should be assessed by a professional.
Bringing In Remote Work
The nature of remote work inherently reduces non-exercise activity thermogenesis (NEAT), our natural, spontaneous movement. Stress levels rise, muscles involuntarily tense, and necessary recovery time is reduced. Over time, the cumulative, unmitigated strain on the spine sets the stage for disc issues.
Disc herniation is, therefore, rarely the result of one sudden, catastrophic movement. It is far more often the result of repeated, unrecovered stress without sufficient protective strength, movement variation, or rest.
How Can Disc Herniation Be Prevented?
Preventing disc herniation does not require an unrealistic pursuit of perfect posture, instead, it requires a focus on consistency and movement variability.
Prioritize movement: Your intervertebral discs rely on the mechanical pumping action of movement to exchange nutrients and stay healthy. Stand up, stretch, or walk briefly every 30 to 45 minutes to cyclically relieve pressure on the spine.
Optimize your setup: Ensure your sitting setup provides adequate lumbar support to maintain the spine's natural curve.
Build a strong support system: Strength is paramount. Developing and maintaining strong core and hip muscles helps distribute load away from the vulnerable spinal segments. Physiotherapy-guided exercises are highly effective for improving spinal stability and reducing vulnerability to repeated strain.
Address early signals: Addressing symptoms early, through rest, movement modification, and professional assessment, significantly improves long-term outcomes and reduces the risk of chronic nerve irritation.
Let's bring it all together, disc herniation is becoming a more common issue, not because people are careless, but because work patterns have drastically changed. The spine responds to what it experiences repeatedly.
Henceforth, be more intentional about protecting the very foundation that allows you to earn, thrive, and remain independent. Your best ergonomic tool is self-awareness.



Comments